An ECG Misdiagnosis - Why 'The Anatomical Approach' Works
Dec 20, 2024This ECG was initially read as Sinus Bradycardia. What are your thoughts?

At first glance the rhythm appears to be a regular bradycardia at a rate of 41 beats per minute, with a QRS morphology consistent with a Right Bundle Branch Block. There seems to be P waves driving each QRS complex. So surely this is a typical Sinus Bradycardia with RBBB, right?
Nope.
I talk a lot about Anchoring Bias. This is the tendency to rely too heavily on the first piece of information received on a topic.
The purpose of ‘The Anatomical Approach to ECG’ is to eliminate/decrease the potential for a missed diagnosis. We don’t want to Anchor prematurely and miss a key finding.
With each step of our Anatomical Approach I want you to ask yourself: How does this change my hypothesis?
Let’s walk through this ECG together.
Step 1 - General Overview of the Rhythm
The rhythm is regularly occurring at a rate of 41 beats per minute. I notice a wide complex QRS throughout the strip. There appear to be P waves driving these wide complex QRS's. For now, this ECG is very undifferentiated, my hypothesis for this regularly occurring bradycardia includes:
- Complete AV Block with Escape Rhythm (ventricular vs junctional with bundle branch block)
- Severe Sinus Bradycardia with bundle branch block
- Fixed Ratio AV Block (2:1, 3:1, etc.) with bundle branch block
Step 2 - Evaluate Atrial Activity
I notice P waves before every QRS complex. These P waves are sharply deflected in V1, which is where I see them best. The P wave axis is slightly deviated to the left, but it appears to be coming from the Sinus Node. The Atrial Rate seems to be higher than the ventricular rate, though. This makes me suspicious for AV Block.
Step 3 - Assess AV Nodal Function
The PR intervals associated with the conducted beats are fixed and within normal limits (120-200ms). As I scan to ensure every P wave conducts to a QRS, I notice that every other P wave is not conducting. This could theoretically represent either Complete AV Block with an Escape rhythm, but more likely represents 2:1 AV Block given the steady PR intervals with the conducted beats.
Step 4 - Ventricular Depolarization
The QRS complex is wide (>120ms). Wide complex QRS's are either due to the beat originating from the ventricles vs. bundle branch block. We previously established that the rhythm seems to be of supraventricular origin (in this case, from the Sinus Node) so I look for typical findings of Right or Left Bundle Branch Blocks. I notice that the Septal "r" wave is preserved in V1 as well as delayed positive forces "R prime" in V1. This is consistent with right sided conduction delay - in this case a Right Bundle Branch Block.
Step 5 - Ventricular Repolarization
The QT Interval, on gross examination, is appropriate for the bradycardic rhythm. There is also appropriate T wave alterations in the setting of a RBBB.
Step 6 - Evaluate for Ischemia & Infarction
I do not notice any focal or diffuse ST segment changes or T wave inversions that are concerning for myocardial injury.
Step 7 - Put it all together
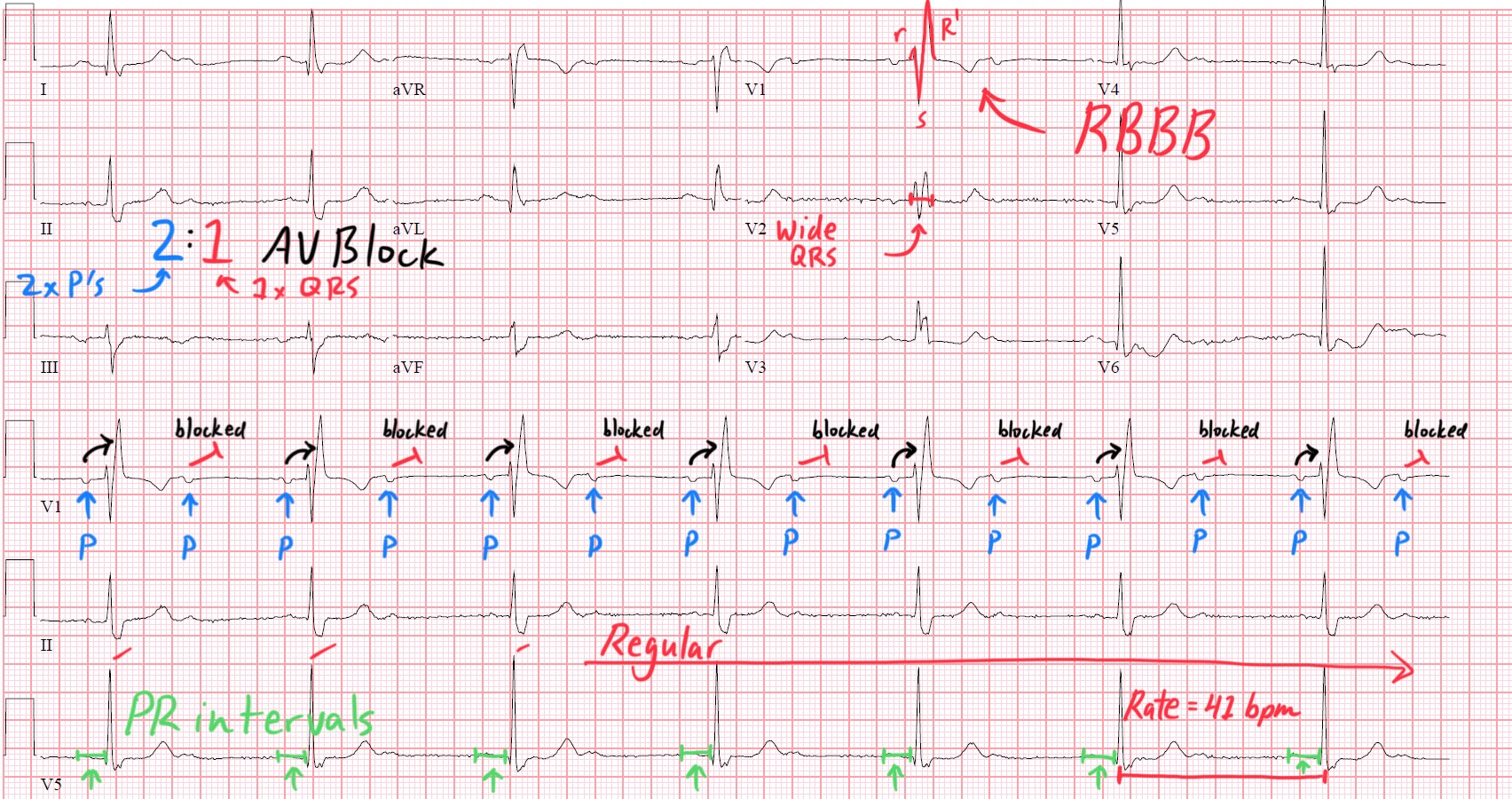
Long story short: Notice how I used a foundation of cardiac electrophysiology as my workflow to arrive at the final diagnosis.
This patient has a potentially lethal rhythm. 2:1 AV Block is at high risk for progressing to an even higher degree block.
As a student one of my mentors would often say: tell me what this isn't and why.
Generating a confident diagnosis isn't always knowing the diagnosis, but rather knowing (with certainty) what the diagnosis ISN'T!
Take care and keep up the great work.
-Reid
ECG Lectures with Reid