The Physiology of Respiratory Sinus Arrhythmia
Jan 17, 2025Respiratory sinus arrhythmia (RSA) is a common and normal ECG finding that reflects the intricate interplay between the respiratory cycle and heart rate. It is most pronounced in young, healthy individuals and is considered a marker of cardiac vagal tone and autonomic nervous system flexibility. This phenomenon showcases how respiration modulates heart rate through the cardiorespiratory coupling of the autonomic nervous system.
In this post, we will explore the physiological mechanism behind RSA, the role of the autonomic nervous system, and how it manifests on the ECG.
What Is Respiratory Sinus Arrhythmia?
Respiratory sinus arrhythmia refers to the cyclical variation in heart rate that occurs with respiration:
- Heart rate increases during inspiration.
- Heart rate decreases during expiration.
This fluctuation is caused by the modulation of vagal (parasympathetic) tone on the sinoatrial (SA) node in response to changes in intrathoracic pressure during the respiratory cycle.
On the ECG, RSA manifests as a regularly irregular rhythm:
- The R-R intervals are shorter during inspiration.
- The R-R intervals are longer during expiration.
The Physiology of Respiratory Sinus Arrhythmia
The mechanism behind RSA is rooted in the dynamic interaction between the cardiovascular and respiratory systems, mediated by the autonomic nervous system. Let’s break it down:
1. Intrathoracic Pressure and Venous Return
During respiration, changes in intrathoracic pressure influence venous return to the heart:
- Inspiration:
- Negative intrathoracic pressure increases venous return to the right atrium.
- This transiently delays blood flow through the pulmonary circuit, reducing left ventricular stroke volume (due to less filling).
- To compensate, the body increases heart rate via reduced vagal tone to maintain cardiac output.
- Expiration:
- Positive intrathoracic pressure decreases venous return to the right atrium.
- Left ventricular stroke volume increases, and vagal tone is restored, slowing the heart rate.
2. Baroreceptor Reflex
- The baroreceptor reflex helps regulate blood pressure and contributes to RSA:
- Baroreceptors in the carotid sinus and aortic arch sense changes in blood pressure during the respiratory cycle.
- Inspiration reduces blood pressure transiently, triggering a reflex decrease in vagal tone and increase in heart rate.
- Expiration increases blood pressure, leading to a reflex increase in vagal tone and decrease in heart rate.
3. Central Autonomic Regulation
The medulla oblongata houses the respiratory and cardiovascular control centers, which are interconnected:
- During inspiration, the activity of the inspiratory neurons inhibits vagal outflow to the heart, increasing heart rate.
- During expiration, vagal activity resumes, slowing the heart rate.
This central coupling between respiratory and cardiovascular centers ensures that heart rate variability aligns with respiratory demands.
4. High-Frequency Modulation of Vagal Tone
RSA is primarily mediated by the parasympathetic nervous system:
- The rapid fluctuations in heart rate during respiration occur due to the fast-acting effects of the vagus nerve on the SA node.
- Sympathetic modulation, which is slower, plays a minimal role in RSA.
Why Is RSA More Pronounced in Healthy Individuals?
The magnitude of RSA reflects the health and adaptability of the autonomic nervous system. It is most pronounced in:
- Young, healthy individuals: They have high parasympathetic tone and flexible autonomic control.
- Athletes: Enhanced vagal tone due to cardiovascular fitness leads to greater RSA.
RSA diminishes in:
- Older adults: Age-related decline in vagal tone and baroreceptor sensitivity reduces RSA.
- Autonomic dysfunction: Conditions like diabetes, heart failure, or neuropathy attenuate RSA.
RSA on the ECG
On the ECG, RSA is evident as cyclical variations in the R-R interval:
- Shortened R-R Intervals During Inspiration: The increased heart rate reduces the time between successive R waves.
- Prolonged R-R Intervals During Expiration: The decreased heart rate lengthens the time between successive R waves.
RSA often results in a regularly irregular rhythm, but it should not be confused with pathological arrhythmias. Careful observation of its correlation with the respiratory cycle confirms the diagnosis.
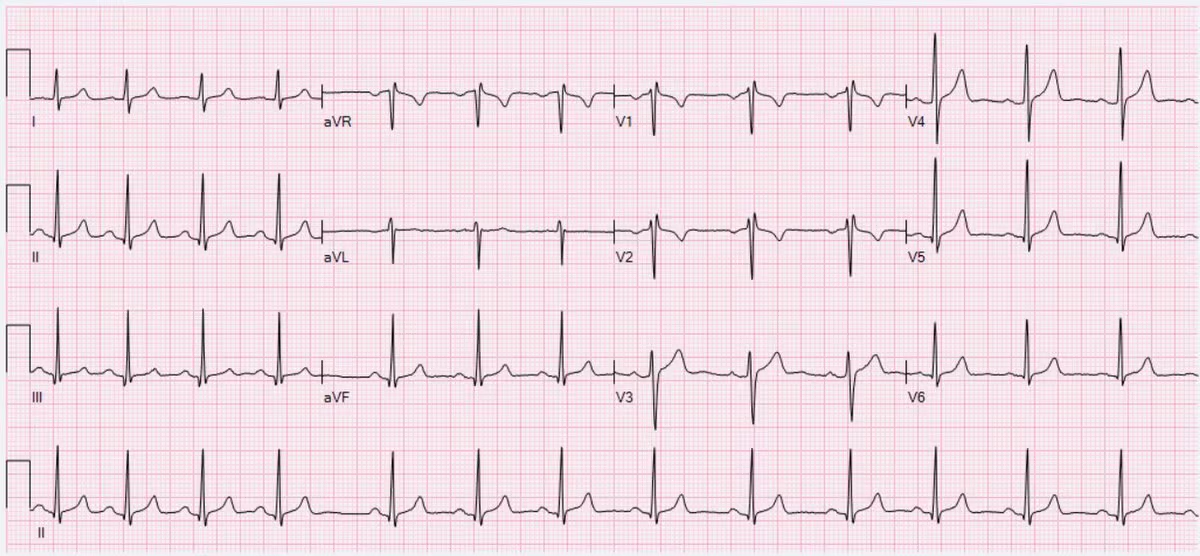
Notice increases and decreases in heart rate associated with intervals consistent with respiration rate (12-20 breaths per minute).
Clinical Significance of RSA
1. Normal Physiologic Finding
- RSA is a marker of autonomic nervous system health and cardiac vagal tone.
- A pronounced RSA is generally a sign of good cardiovascular fitness and autonomic flexibility.
2. Diagnostic Applications
- Autonomic Testing: RSA is used as a non-invasive measure of parasympathetic function, particularly in conditions like diabetes or autonomic neuropathy.
- Pediatric Cardiology: In children, RSA can be exaggerated and should not be mistaken for an arrhythmia.
3. Conditions with Reduced RSA
- Aging
- Heart failure
- Autonomic dysfunction (e.g., diabetic autonomic neuropathy)
- Chronic stress or sympathetic overactivity
Clinical Pearl: Distinguishing RSA from Pathological Arrhythmias
While RSA causes an irregular rhythm, it should not be mistaken for arrhythmias such as atrial fibrillation or sinus arrhythmia due to conduction abnormalities. Key differentiators include:
- Association with Respiration: RSA is tightly linked to the respiratory cycle, whereas pathological arrhythmias are not.
- P-Wave Morphology: In RSA, normal sinus P waves precede each QRS complex.
Hope this helps! Take care.
-Reid
ECG Lectures with Reid