Understanding Atrial Flutter: A Deep Dive into Typical and Atypical Reentry Circuits
Jan 10, 2025Atrial flutter is a macro-reentrant atrial tachycardia defined by organized atrial activity and rapid atrial rates, typically between 250 and 350 beats per minute. While atrial flutter is often grouped into a single category, it is essential to distinguish between its typical and atypical forms. These distinctions are based on the location and characteristics of the reentry circuit within the atria, which have implications for diagnosis, management, and ablation strategies.
Let’s explore the key differences between typical and atypical atrial flutter, focusing on the anatomy and physiology of their reentry circuits.
The Concept of Reentry in Atrial Flutter
At the core of atrial flutter is a macro-reentrant circuit—a self-sustaining electrical loop that propagates through a fixed path within the atrium. For reentry to occur, the circuit requires:
1. A circuit path: A defined route for the impulse to travel.
2. Unidirectional block: A region of impaired conduction that forces the impulse to take a specific route.
3. Conduction delay: A delay in the circuit that allows for recovery of the tissue ahead of the impulse, ensuring continued propagation.
Typical Atrial Flutter: The Right Atrial Cavotricuspid Circuit
- Anatomy of the Circuit
- Location: The reentry circuit in typical atrial flutter revolves within the right atrium, centered around the tricuspid valve annulus.
- Key Structures:
- Cavotricuspid isthmus (CTI): A critical component of the circuit. This isthmus is the narrow region of tissue between the inferior vena cava (IVC) and the tricuspid valve.
- Other boundaries: The crista terminalis, Eustachian ridge, and atrial walls help define the circuit.
Forms of Typical Atrial Flutter
1. Counterclockwise Flutter (Most Common):
- The impulse travels counterclockwise around the tricuspid annulus.
- On the ECG:
- Negative flutter waves in inferior leads (II, III, aVF).
- Positive flutter waves in lead V1.
- This is the classic form of atrial flutter.
2. Clockwise Flutter (Reverse Typical Flutter):
- The impulse travels clockwise around the tricuspid annulus.
- On the ECG:
- Positive flutter waves in inferior leads.
- Negative flutter waves in lead V1.
Why Is the CTI Important?
The CTI serves as a modifiable target during catheter ablation. By creating a line of block in the CTI, the reentry circuit is interrupted, rendering the flutter non-sustainable.
Atypical Atrial Flutter: Beyond the CTI Circuit
Unlike typical atrial flutter, atypical flutter does not depend on the cavotricuspid isthmus. Instead, it involves reentry circuits located in various regions of either atrium, often associated with structural heart disease or prior atrial surgery.
Anatomy of the Circuit
Atypical atrial flutter circuits are more diverse and occur in areas of scar tissue, fibrosis, or surgical/anatomical barriers. Common locations include:
1. Left Atrium:
- Common after atrial fibrillation (AF) ablation procedures or left atrial surgery.
- Circuit paths may involve:
- Pulmonary vein isolation scars.
- Mitral annulus (peri-mitral flutter).
- Roof or floor of the left atrium.
2. Right Atrium:
- Typically seen after congenital heart defect repair (e.g., atrial septal defect or Fontan procedures).
- Circuits may form around surgical scars or suture lines.
Key Features of Atypical Flutter
- Highly Variable ECG Morphologies:
- The location of the circuit determines the flutter wave pattern.
- No consistent pattern like the sawtooth waves of typical flutter.
- Slower Rates:
- Atypical flutter often has atrial rates closer to 200–250 bpm due to larger or more complex reentry circuits.
Distinguishing Typical vs. Atypical Flutter
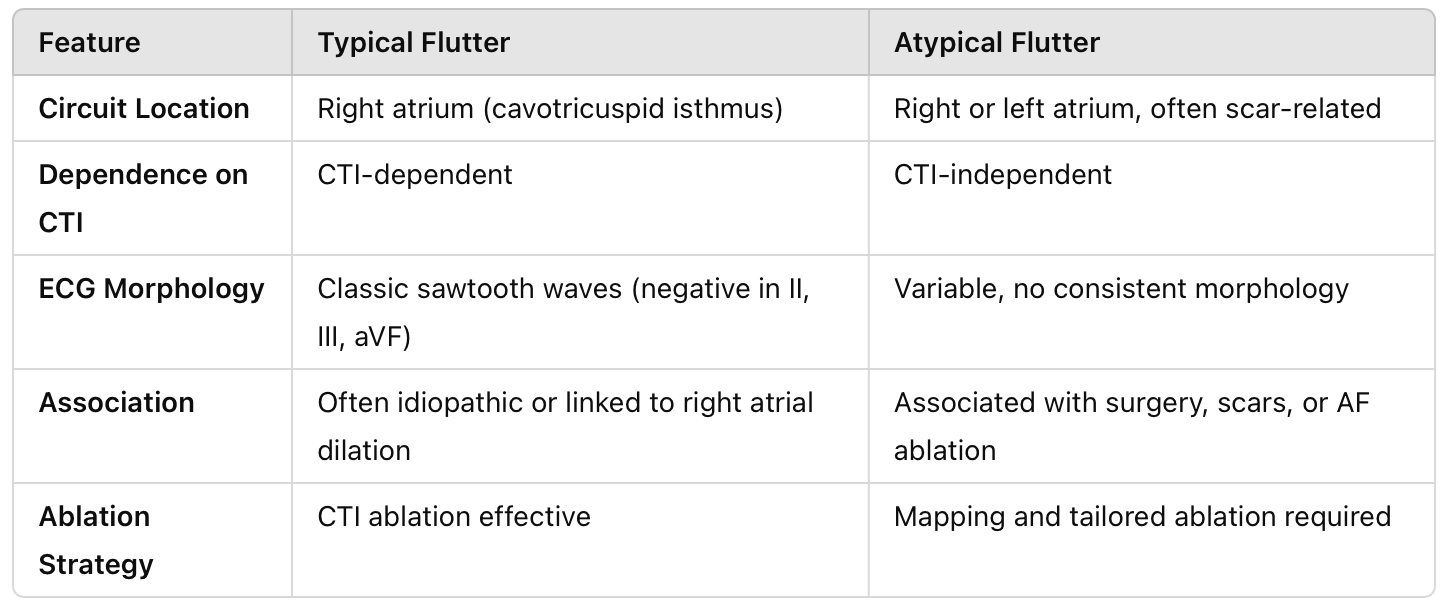
Why Does the Type of Atrial Flutter Matter?
1. Treatment Strategy:
- Typical flutter is easily managed with CTI ablation, which has high success rates (>95%).
- Atypical flutter requires detailed mapping to identify the circuit, which can be complex and time-consuming.
2. Associated Conditions:
- Typical flutter is often seen in conditions that dilate the right atrium, such as pulmonary hypertension or chronic obstructive pulmonary disease.
- Atypical flutter is usually secondary to structural heart disease or prior interventions (e.g., AF ablation scars).
3. Risk of Recurrence:
- Atypical flutter has a higher likelihood of recurrence due to its association with underlying atrial pathology.
Management Overview
1. Rate Control:
- Beta-blockers or calcium channel blockers can help control ventricular rates during atrial flutter.
- Digoxin is less effective, particularly in high adrenergic states.
2. Rhythm Control:
- Cardioversion: Both typical and atypical flutter are highly responsive to synchronized cardioversion.
- Antiarrhythmic Drugs: Class IC (e.g., flecainide) or Class III agents (e.g., amiodarone) may be effective, though ablation is preferred.
3. Catheter Ablation:
- Typical flutter: Ablation of the CTI is the gold standard.
- Atypical flutter: Requires detailed electroanatomic mapping to identify and ablate the specific circuit.
4. Anticoagulation:
- Stroke risk is similar to atrial fibrillation and should be assessed using the CHA₂DS₂-VASc score.
Key Takeaways
- Typical atrial flutter involves a predictable, CTI-dependent reentry circuit in the right atrium and has a classic sawtooth ECG pattern.
- Atypical atrial flutter is more complex, often involving scars, fibrosis, or prior interventions, and requires advanced mapping for ablation.
- Recognizing the type of atrial flutter is essential for tailoring management strategies, particularly when considering catheter ablation.
Hope this helps!
-Reid
ECG Lectures with Reid